Documentation Shapes Every Visit.
Finish Clinical Notes During the Visit
Delayed notes slow billing, follow-ups, and care decisions. Vozo keeps documentation clear, complete, and finished during the visit.






Why Choose Vozo for Notes & Documentation
Built for clinicians who document during care, not after hours.

Built for visits
Supports fast-moving outpatient encounters without disrupting patient interaction.

Cleaner documentation
Structured notes reduce missing details and downstream clarification work.

Cross-specialty ready
Works consistently across behavioral health, primary care, pediatrics, and specialties.
Features
What Notes & Documentation Handles for You
Keeps clinical notes accurate, consistent, and ready for care continuity.
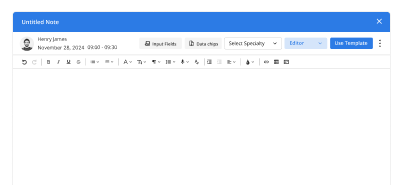
Structured Notes
Create clear EHR clinical notes using consistent formats across visits and providers.

Clinical Notes Templates
Use specialty-specific templates that reduce typing and standardize documentation.
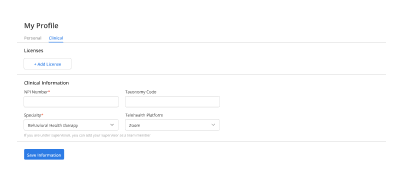
Faster Completion
Healthcare documentation tools streamline charting without disrupting patient interaction.
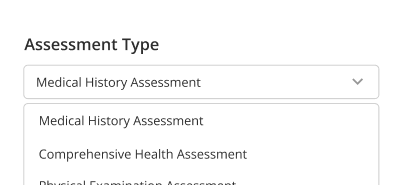
Assessment & Progress Notes
Document evaluations, follow-ups, and outcomes in one continuous clinical record.
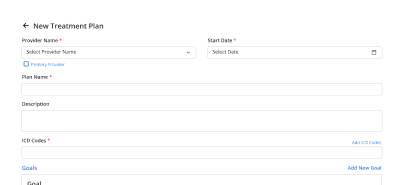
Care Alignment
Notes stay aligned with treatment plans, orders, and care coordination workflows.
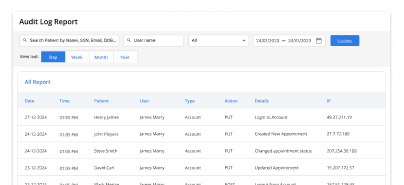
Compliance support
Documentation follows clinical and regulatory standards without extra effort.
How Notes & Documentation Fit Into Your Day
![]() Post-visit charting
Post-visit charting
![]() Note completion
Note completion
![]() Team handoffs
Team handoffs
![]() Billing alignment
Billing alignment
![]() Patient engagement
Patient engagement
![]() Day-end predictability
Day-end predictability
![]() Documentation accuracy
Documentation accuracy
Operational Impact You Can Measure
Ready to see how documentation could feel lighter?
Additional Related Features
Testimonials
Success Stories From Our Users
What Practices Say
“Vozo helped me complete patient notes with less end-of-day catch-up. Templates, visit details, and follow-up items stay organized, so documentation feels easier to finish during the actual care workflow.”
— Dr. Alden Pierce, Family Medicine Physician
“Our providers needed a cleaner way to manage clinical documentation without slowing down appointments. Vozo made notes easier to structure, review, and complete across busy clinic days.”
— Mira Langford, Clinical Documentation Manager
Blogs & Resources
Resources to Help Your Practice Grow
CCM Workflow Automation
Automates monthly tasks, notes, and billing for Chronic Care Management, ensuring compliance and freeing staff for patient care.
AI-Powered EHR Documentation
AI transforms EHR charting with voice-to-text and smart templates, accelerating clinical notes for better efficiency.
Manual SOAP Notes Burnout
Traditional SOAP notes exhaust mental health providers; discover streamlined alternatives for behavioral health documentation.
FAQ
What Providers Ask Us Most about Clinical Documentation
Most clinicians spend nearly a third of their day entering data, updating records, and completing notes after hours. Without structured clinical documentation tools and smart templates, every encounter becomes a manual task, pulling providers away from direct patient care and increasing the risk of documentation errors and burnout.
AI charting tools capture structured patient data from the encounter and auto-populate EHR fields, eliminating manual typing between visits. Voice-to-text transcription and smart note generation reduce clinical documentation time significantly, letting providers review and finalize notes in seconds rather than spending hours on after-hours charting.
Progress notes document the diagnosis, treatment plan, and clinical outcomes, forming part of the official medical record used for billing and provider communication. Psychotherapy notes are private clinical reflections stored separately with stronger legal protections, and a compliant EHR clinical documentation system keeps both clearly distinguished and securely accessible.
Pre-built SOAP and DAP templates structure documentation so every provider captures the same data elements in the same order, reducing omissions, improving audit readiness, and speeding up note completion. Consistent medical note templates also make it easier to track patient progress and support accurate coding during billing.
Macros auto-populate repetitive text blocks with a single shortcut, while data chips instantly insert patient-specific variables like name, diagnosis, and medications directly into the note. These EHR documentation tools cut manual typing, reduce transcription errors, and ensure notes stay accurate, consistent, and compliant without slowing the clinical workflow.
Vozo’s notes and documentation tools include macros, data chips, and rich text formatting, all accessible from one clean charting workspace.
Yes. Specialty-specific clinical documentation requires different data fields, exam structures, and follow-up logic than general medicine. A flexible EHR lets providers build and save custom note templates tailored to their specialty, whether behavioral health, internal medicine, or orthopedics, so documentation matches how care is actually delivered, not a generic default.
Notes completed during or immediately after the encounter capture the most accurate clinical detail, directly supporting the service codes submitted on the claim. Delayed documentation increases the risk of missed diagnoses, undercoding, or audit flags. EHR medical documentation tools that prompt real-time note completion improve both compliance and reimbursement outcomes.
Yes. In Vozo, completed clinical notes flow directly into the billing workflow with diagnosis codes, CPT codes, and service details linked from the encounter documentation. This eliminates duplicate data entry between clinical and billing teams, reduces claim errors, and supports faster, cleaner reimbursement from the moment a note is finalized.
Vozo starts at just $25 per provider per month, with full access to clinical documentation, note templates, AI charting, macros, and billing integration included from day one. A 14-day free trial is also available with no credit card required, and a guided demo can be scheduled for practices wanting a live walkthrough before going live.
Stop carrying charts home. Complete accurate documentation while the visit is still fresh.
✓ No Credit Card Required
- 24/7 Support
- Free data migration from your old EHR
- Built-in telehealth
- Automated appointment reminders
- Increase revenue by 30%
- Complete patient notes