Coverage Before Check-In.
EHR with Insurance Billing That Prevents Claim Delays
Insurance errors and manual follow-ups slow revenue; Vozo connects eligibility, claims, and billing into one reliable workflow.






Why Choose Vozo for Insurance Billing
Built for outpatient practices that need insurance workflows to work reliably every day.

Coverage Clarity Upfront
Insurance eligibility verification EHR checks reduce last-minute surprises that slow visits and frustrate patients.

Claims Built from Care
The claims processing EHR platform links documentation, codes, and billing automatically.

Less Manual Chasing
Automated insurance verification software cuts repetitive calls and payer follow-ups.
Features
What Vozo Insurance Handles For You
Keeps insurance workflows moving smoothly from intake through claim resolution.
Eligibility Verification
Confirms active coverage before visits to prevent denials, delays, and front-desk confusion.
Claim Creation
Builds claims directly from visit documentation to reduce manual entry and missing information.
Claim Submission
Submits claims inside the EHR without exporting data or switching billing systems.
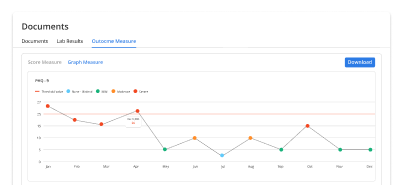
Status Tracking
Shows real-time claim progress so teams stop chasing payers blindly.
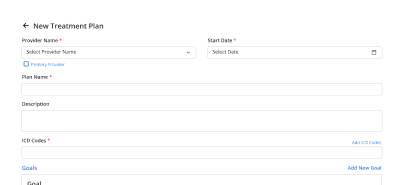
Error Prevention
Flags incomplete or mismatched claim details before submission to reduce rework.
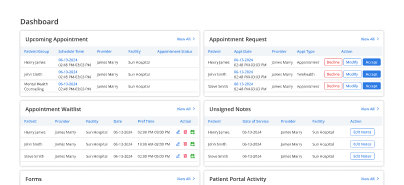
Billing Continuity
Keeps insurance and payment workflows connected through posting and reconciliation.
How Insurance Fits Into Your Day
![]() Eligibility confidence
Eligibility confidence
![]() Smoother check-ins
Smoother check-ins
![]() Cleaner claims
Cleaner claims
![]() Fewer billing callbacks
Fewer billing callbacks
![]() Clear claim visibility
Clear claim visibility
![]() Faster closeouts
Faster closeouts
![]() Predictable revenue
Predictable revenue
Operational Impact You Can Measure
Clear insurance workflows reduce rework, shorten billing cycles, and improve day-to-day financial predictability.
Additional Related Features
Billing & Payments
Faster posting ➜
Dedicated Dashboard
Claims visibility ➜
Documentation
Cleaner coding ➜
Reporting
Billing clarity ➜
Testimonials
Success Stories From Our Users
What Practices Say
“Eligibility issues stopped derailing our front desk once everything lived in one place.”
— Practice Manager, Multi-Provider Clinic
“Claims are cleaner because billing and documentation finally match.”
— Billing Lead, Private Practice
Blogs & Resources
Resources to Help Your Practice Grow
Prior Authorization Essentials
Explains process, purposes like medical necessity/cost control, and benefits for providers, insurers, and patients.
Eligibility Verification Steps
The essential five-step process confirms patient insurance, reducing billing errors and accelerating reimbursements.
Automation Efficiency Gains
Smart tools reduce insurance processing time by 70% via automated verification and prior authorization workflows.
FAQ
What Care Teams Ask About Insurance Billing And Claims
Insurance billing is native to the Vozo EHR and does not require external systems. All workflows operate inside the platform.
Eligibility is verified before the visit using integrated workflows. This reduces denials and front-desk disruptions.
Claims are submitted directly from the EHR without duplicate data entry. Documentation and billing remain connected.
Vozo is designed for small to mid-sized outpatient practices. Workflows remain manageable as volume increases.
Insurance workflows integrate directly with Vozo billing features. Claims and payments stay aligned throughout the process.
Keep coverage, claims, and billing aligned before issues interrupt your team’s day.
✓ No Credit Card Required
- 24/7 Support
- Free data migration from your old EHR
- Built-in telehealth
- Automated appointment reminders
- Increase revenue by 30%
- Complete patient notes